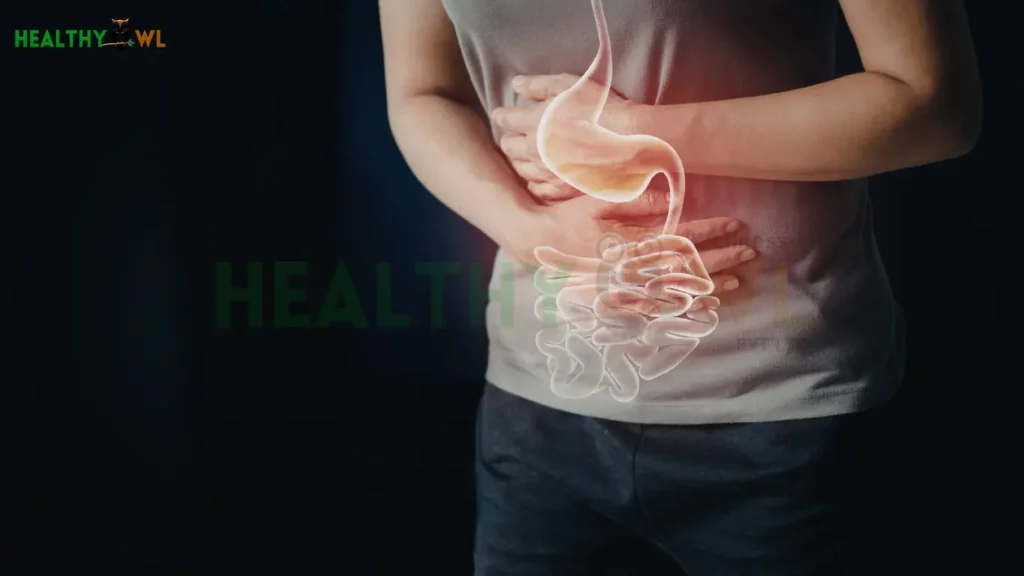
You switched to vibrant kale salads. You swapped your morning bagel for chia seed pudding. You’ve embraced the world of sprouts, oats, and green smoothies. By all accounts, you should feel like a superhero.
So, why are you so bloated? i
I you’re experiencing digestive problems from healthy eating, you aren’t “broken,” and your body isn’t rejecting nutrition. You’re likely experiencing Gut Overload. While “clean” foods are packed with nutrients, they can also be taxing on a digestive system that isn’t prepared for the sudden shift.
Let’s dive into the science of why your healthy habits might be causing temporary havoc and how to fix it without going back to processed junk.
Why “Clean” Food Can Cause Messy Digestion
When you overhaul your diet, your microbiome (the trillions of bacteria in your gut) undergoes a massive transition. Most digestive distress in “new” healthy eaters stems from these five common culprits:
1. The Fiber “Flash Flood”
Fiber is the holy grail of gut health, but your body treats it like a workout. According to the Academy of Nutrition and Dietetics, adult women need approximately 25g and men 38g of fiber daily. However, jumping from 10g to 30g overnight can cause a “fermentation surge.”
Most digestive distress stems from these common culprits:
Soluble vs. Insoluble Fiber: Understanding the Difference
Not all fiber behaves the same way in your gut. According to research by Slavin JL (2013), differentiating between the two is key to managing bloating:
- Soluble Fiber (Oats, Chia, Lentils): This fiber dissolves in water to form a gel-like substance. It ferments quickly in the colon, producing Short-Chain Fatty Acids (SCFAs) like butyrate, acetate, and propionate. While SCFAs are vital for health, rapid fermentation can lead to immediate gas.
- Insoluble Fiber (Raw Greens, Bran, Skin of fruit): This does not dissolve in water. It adds bulk to the stool and speeds up transit time. If your gut is sensitive, too much insoluble fiber can feel like “sandpaper” on your intestinal lining, causing discomfort.
2. The Raw Food Struggle
Raw vegetables, especially cruciferous ones like broccoli, cauliflower, and kale, contain cellulose and insoluble fiber. These are structurally tough. If you have low stomach acid or a sensitive gut lining, your body may struggle to “mechanically” break these down, leading to undigested food sitting in the gut. Experts like The Gut Health Doctor suggest that cooking acts as a form of “pre-digestion,” making these fibers gentler on the colon.
3. Hidden FODMAP Sensitivities
Even “superfoods” like garlic, onions, apples, and lentils contain fermentable short-chain carbohydrates known as FODMAPs. According to research from Monash University, these carbs pull water into the intestine and ferment rapidly. For those with sensitive systems, this is a primary trigger for IBS-like symptoms.
4. The “Kitchen Sink” Smoothie
Smoothies are convenient, but they often lead to Digestive Stacking. When you blend spinach, protein powder, nut butter, flax seeds, and fruit, you are consuming a massive caloric and fiber load in seconds. Because you aren’t chewing, you skip the first step of digestion (salivary enzymes), hitting your stomach with a “nutrient bomb” it can’t keep up with.
5. Underlying Microbiome Imbalances
Sometimes, healthy food acts as a spotlight for existing issues. Conditions like SIBO (Small Intestinal Bacterial Overgrowth) or Leaky Gut can make even the healthiest lentil soup feel like a poison.
Signs Your Gut Is Overloaded
How do you know if it’s the food or the amount of food? Watch for these red flags:
- The “Food Baby”: Extreme bloating that progressively gets worse toward the evening.
- Brain Fog: Feeling sluggish or “heavy-headed” shortly after a high-fiber meal.
- Transit Trouble: Constipation despite high fiber intake (usually due to lack of water) or sudden loose stools after eating raw greens.
Probiotics & Supporting Your Gut Bacteria
Your gut is an ecosystem. If you introduce high-fiber foods without the right “workforce” (bacteria) to process them, you will experience distress.
- Introduce Probiotics Gradually: Fermented foods like curd, buttermilk, or sauerkraut introduce live beneficial bacteria. However, starting with large amounts can actually increase bloating initially.
- Prebiotics are the Fuel: Fiber is the food for your bacteria. To support a healthy microbiome, you need to provide fiber (prebiotics) and live cultures (probiotics) in a balanced ratio.
- Diversity is Key: A study in Nature Reviews Gastroenterology & Hepatology explains that a diverse diet leads to a diverse microbiome, which is more resilient to dietary changes.
How to Fix Your Digestion (Without Quitting Your Diet)
You don’t have to choose between health and comfort. Use these science-backed strategies to find the middle ground.
Step 1: The “Low and Slow” Fiber Method
Don’t double your fiber intake in 24 hours. Add 5 grams of fiber per week. This allows your bacterial colonies to grow in proportion to the “food” you’re giving them.
Step 2: The Power of Heat (Cook Your Greens)
If raw salads make you bloat, steam, sauté, or roast your vegetables. Cooking initiates the breakdown of tough fibers and neutralizes certain anti-nutrients, making the vitamins more bioavailable and the fiber gentler on your colon.
Step 3: Master the “Art of the Chew”
Digestion begins in the brain and the mouth. Aim for 20–30 chews per bite. Chewing breaks down cell walls in plants and mixes food with salivary amylase, significantly reducing the workload on your small intestine.
Step 4: Use “Digestive Fire” Spices
Incorporate carminative herbs that help expel gas and stimulate enzymes:
- Ginger: Speeds up gastric emptying.
- Cumin & Ajwain: Traditional remedies for reducing flatulence.
- Fennel: Relaxes the intestinal muscles.
Step 5: Hydrate, Hydrate, Hydrate
Fiber is a sponge. If you eat a high-fiber diet without drinking enough water, that fiber will turn into “bricks” in your digestive tract, leading to painful constipation.
When to Seek Professional Help
If you’ve tried the tips above for 3 weeks and still feel miserable, it may be time to look deeper. Consult a professional if you experience:
- Unexplained weight loss.
- Blood in the stool.
- Chronic pain that interrupts sleep.
- Persistent diarrhea.
Reclaiming Your Gut Health with Healthy Owl Wellness
At Healthy Owl Wellness, we understand that “healthy” isn’t a one-size-fits-all label. If your new diet is making you feel worse, we specialize in helping you bridge the gap.
Our experts focus on personalized gut repair protocols and hormone balance to ensure your body can actually absorb the nutrients you’re feeding it. We don’t believe in restrictive fads—we believe in science-based, sustainable lifestyle changes.
Ready to stop the bloating? Book your consultation with Healthy Owl Wellness today.
Frequently Asked Questions
1. Why do I get bloated after eating healthy food?
It’s usually due to a sudden increase in fiber or a sensitivity to FODMAPs. Your gut bacteria produce gas as they ferment new fibers they aren’t used to yet.
2. Can too much fiber cause constipation?
Yes. Fiber needs water to move. If you increase fiber without increasing hydration, it can lead to a “backup” in your system.
3. Why do salads upset my stomach but cooked veggies don’t?
Cooking breaks down the tough cellulose and fibers in vegetables, essentially “pre-digesting” them so your stomach doesn’t have to work as hard.
4. How long does it take for the gut to adjust to a new diet?
Most people see a significant reduction in gas and bloating within 14 to 21 days as the microbiome stabilizes.
Sources & References
- Fiber Guidelines: Academy of Nutrition and Dietetics. “Position of the Academy of Nutrition and Dietetics: Health Implications of Dietary Fiber.”
- Microbiome Adaptation: Nature Reviews Gastroenterology & Hepatology. “High-fiber dietary intervention alters the human gut microbiome.”
- FODMAP Science: Monash University. “The Low FODMAP Diet for Irritable Bowel Syndrome.”
- IBS & Gut Health: NIDDK (National Institute of Diabetes and Digestive and Kidney Diseases). “Symptoms & Causes of IBS.”
- Digestion Techniques: UCSF Health. “Patient Education: Increasing Fiber Intake.”